Non-Peptide GLP-1 Agonist
The First Truly Orally Bioavailable GLP-1 Agonist: 20-40% Absorption Without Restrictions
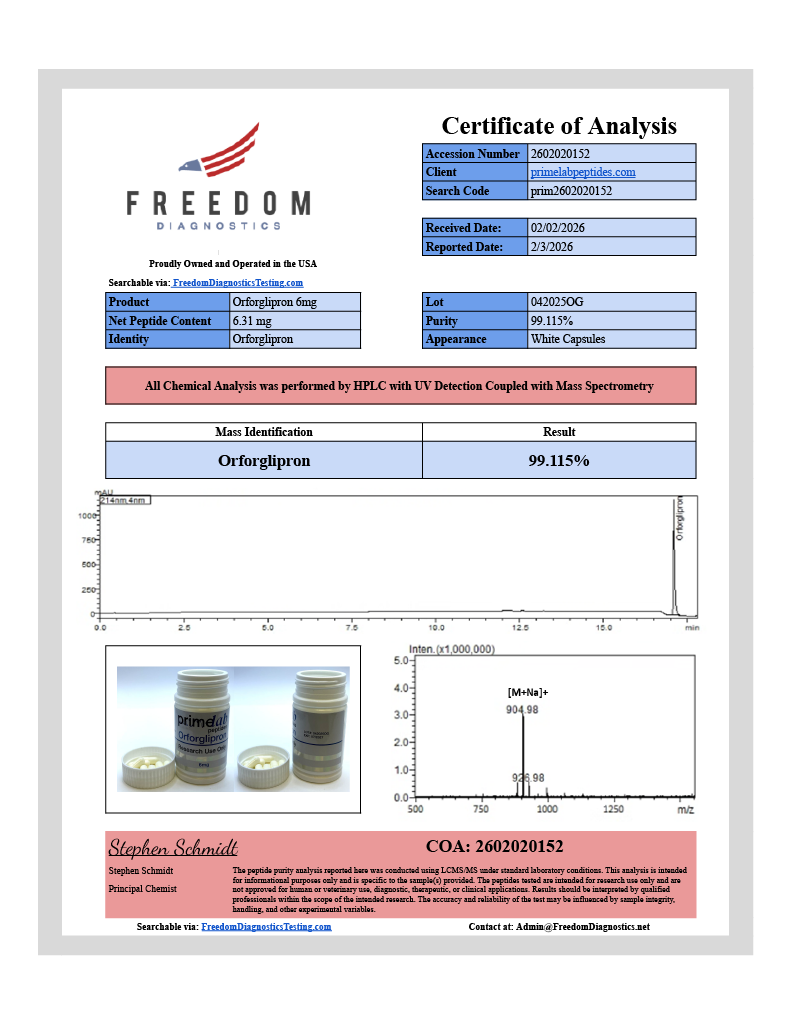
Orforglipron (LY3502970) is a non-peptide, small-molecule partial agonist of the GLP-1 receptor with unprecedented oral bioavailability. While oral semaglutide achieves just 0.4-1% absorption requiring fasting and absorption enhancers, Orforglipron demonstrates 20-40% bioavailability in cynomolgus monkeys — with no food restrictions. Clinical trials show weight loss of 8.6-14.7% over 26-36 weeks, with A1c reductions up to 2.1%.
- 20-40% oral bioavailability (vs 0.4-1% for oral semaglutide)
- No fasting requirements or absorption enhancers needed
- Once-daily oral administration
- Weight loss: 8.6-14.7% over 26-36 weeks
- A1c reduction: up to 2.1% over 26 weeks
For laboratory research use only. Not for human consumption.

Biased Agonism
G-Protein Signaling Without β-Arrestin: Why Orforglipron Resists Desensitization
Orforglipron's unique mechanism lies in its biased agonism. Its activity is characterized primarily by cAMP signaling (G-protein coupled) with minimal β-arrestin recruitment. The cAMP pathway drives all desired GLP-1 effects: glucose metabolism, gastric slowing, satiety, and beta-cell protection. β-arrestin causes receptor desensitization (tachyphylaxis) — by avoiding this pathway, Orforglipron maintains efficacy without requiring dose escalation or treatment breaks.
- Biased toward G-protein (cAMP) signaling
- Minimal β-arrestin recruitment
- Reduced risk of tachyphylaxis (desensitization)
- No dose escalation required for sustained effects
- Unique binding pocket on GLP-1 receptor
For laboratory research use only. Not for human consumption.

Multi-System Benefits
From Beta-Cell Protection to Cardiovascular Risk: Comprehensive Metabolic Research
Beyond weight and glucose, Orforglipron research reveals profound effects on cardiovascular and inflammatory markers. Clinical data shows LDL reduction of 3.7-14.3%, triglycerides down 8.4-16.6%, and ApoB (the primary driver of atherosclerosis) reduced by 8.3-12.2%. CRP levels — a key inflammation marker — dropped 26-39.3%. Crucially, GLP-1 stimulation promotes beta-cell survival and proliferation, making it one of the only known mechanisms for potentially reversing diabetes pathology.
- Beta-cell protection: Prevents apoptosis, promotes new cell growth
- LDL cholesterol: -3.7% to -14.3%
- Triglycerides: -8.4% to -16.6%
- ApoB (atherosclerosis driver): -8.3% to -12.2%
- CRP (inflammation marker): -26% to -39.3%
- No significant hypoglycemia risk
For laboratory research use only. Not for human consumption.

The Science Behind Oral GLP-1 Innovation: Why Orforglipron Changes Everything
Orforglipron (LY3502970, OWL833) represents a fundamental breakthrough in incretin research. As a non-peptide, small-molecule partial agonist of the GLP-1 receptor, it overcomes the two critical limitations that have constrained GLP-1 therapeutics: poor oral bioavailability and receptor desensitization. Where oral semaglutide achieves just 0.4-1% absorption requiring fasting and absorption enhancers, Orforglipron demonstrates 20-40% bioavailability with no food restrictions — the first truly practical oral GLP-1 agonist.
The mechanism is elegantly biased. Orforglipron's activity is characterized primarily by cAMP signaling (G-protein coupled receptor activity) with minimal β-arrestin recruitment. This distinction matters: cAMP activation drives all the beneficial GLP-1 effects — glucose metabolism, gastric slowing, satiety signaling, and beta-cell protection. β-arrestin, by contrast, causes tachyphylaxis (receptor desensitization), requiring dose escalation or treatment breaks. By avoiding β-arrestin, Orforglipron maintains efficacy long-term.
Clinical evidence is substantial. Phase 2b trials show weight loss of 8.6-14.7% over 26-36 weeks (average 16 pounds over 40 weeks), with waist circumference reductions averaging 5.32 cm. A1c levels dropped up to 2.1% — significantly more effective than metformin or dulaglutide. Fasting glucose decreased 23-44 mg/dL. Critically, no significant hypoglycemia risk was observed, a common limiting factor in diabetes treatment.
Cardiovascular and inflammatory benefits extend beyond weight loss. LDL dropped 3.7-14.3%, triglycerides 8.4-16.6%, and ApoB (the primary driver of atherosclerotic plaque) 8.3-12.2%. HDL increased in many subjects. CRP levels — a systemic inflammation marker — decreased 26-39.3%, with implications for arthritis, neurodegenerative disorders, wound healing, and longevity research. These benefits occur even in non-obese individuals, confirming effects independent of weight loss.
For research teams investigating metabolic syndrome, diabetes pathophysiology, cardiovascular risk, inflammation, or GLP-1 receptor biology, Orforglipron provides an unprecedented tool: a stable, orally bioavailable, desensitization-resistant GLP-1 agonist with comprehensive human trial data across multiple metabolic endpoints.
For research use only. Not for human consumption.
References
- Kim MK, Kim HS. An Overview of Existing and Emerging Weight-Loss Drugs to Target Obesity-Related Complications. Biomol Ther (Seoul). 2025;33(1):5-17.
- Lütkemeyer C et al. Effects of once-daily oral orforglipron on weight and metabolic markers: a systematic review and meta-analysis. Arch Endocrinol Metab. 2024;68:e230469.
- Kawai T et al. Structural basis for GLP-1 receptor activation by LY3502970, an orally active nonpeptide agonist. PNAS. 2020;117(47):29959-29967.
- Pratt E et al. Orforglipron (LY3502970), a novel, oral non-peptide GLP-1 receptor agonist: A Phase 1a study in healthy participants. Diabetes Obes Metab. 2023;25(9):2634-2641.
- Ma X et al. Effect of Food Consumption on the Pharmacokinetics of Orforglipron. Diabetes Ther. 2024;15(4):819-832.
- Dutta D et al. Orforglipron, a novel non-peptide oral daily GLP-1 receptor agonist as an anti-obesity medicine: A systematic review. Obes Sci Pract. 2024;10(2):e743.
- Karakasis P et al. Safety and efficacy of orforglipron and danuglipron for type 2 diabetes and obesity: systematic review and meta-analysis. Metabolism. 2023;149:155710.
- Wharton S et al. Orforglipron is associated with improvements of CV risk biomarkers in participants with type 2 diabetes or obesity. Cardiovasc Diabetol. 2025;24(1):240.